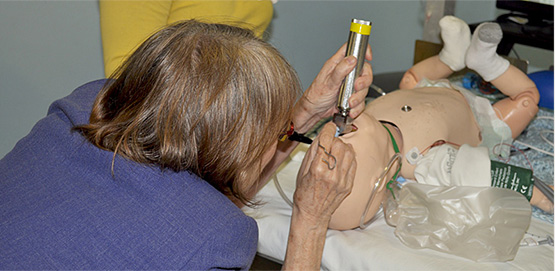
Training
Emergency room doctors spend only 16 percent of their training time learning how to recognize and respond to pediatric emergencies — yet up to 33 percent of their patients are babies and children.
That’s why R Baby partners with leading medical schools and hospitals to fund programs that bring essential training directly to physicians and ER staff, from life-like emergency simulations to education modules, vital signs awareness and other innovative programs.
Scroll down to learn more about our projects:
R Baby’s Grants Train:
- Primary Care Physicians
- Family Medicine Doctors
- General and Pediatric Attending ER Physicians
- Fellows and Resident Doctors
- Nurse Practitioners
- Physician Assistants
- Nurses
- Medics and EMTs
- Technicians
- Respiratory Therapists
- Pharmacists